🏠 Stay at home! 25% discount on all medicines
Can You Take Adderall While Pregnant or Breastfeeding? A Comprehensive Guide

When it comes to medication use during pregnancy and breastfeeding, many mothers find themselves in a dilemma, seeking to balance their health needs with the well-being of their baby. One medication that often raises questions is Adderall, a prescription drug widely used to treat Attention Deficit Hyperactivity Disorder (ADHD). The primary components of Adderall—dextroamphetamine and amphetamine—have been shown to effectively manage ADHD symptoms, but their safety during pregnancy and lactation remains a topic of heated discussion. In this article, we will delve into whether it is safe to take Adderall while pregnant or breastfeeding, examining current research and expert recommendations to provide a comprehensive perspective.
Over the years, various studies have emerged regarding the effects of psychostimulants, including Adderall, on pregnancy outcomes and infant development. Notably, concerns have arisen regarding the potential risks of these medications, which can cross the placenta and enter breast milk. Pregnant women and new mothers with ADHD face unique challenges as they navigate their treatment options amidst these health concerns. The information provided here will empower mothers-to-be and breastfeeding mothers to make informed choices about their health care.
In understanding the implications of using Adderall while pregnant or breastfeeding, we will explore the risks associated with its use, the available evidence from recent studies, and the necessary steps to take if you find yourself in this situation. Whether you are considering taking Adderall to manage your ADHD symptoms or weighing your options after discovering you are pregnant, this guide will furnish you with essential insights to navigate this critical phase of your life.

Understanding Adderall: What Is It and How Does It Work?
Before discussing the implications of taking Adderall during pregnancy and breastfeeding, it is essential to understand what the medication is and how it works in the body. Adderall is a combination of two stimulant medications, dextroamphetamine and amphetamine, which function by increasing the levels of certain neurotransmitters in the brain. These neurotransmitters, primarily dopamine and norepinephrine, play a crucial role in regulating attention, impulse control, and hyperactivity.
For individuals with ADHD, Adderall can enhance focus and concentration by helping to mitigate the overwhelming symptoms of the condition. However, while effective for many, the use of stimulants also comes with potential side effects, including increased heart rate, anxiety, and insomnia. In healthy adults, these effects can be manageable, but their implications can change dramatically during pregnancy and lactation.
The effectiveness of Adderall is well-documented; however, it is important to approach its use cautiously, especially for pregnant or breastfeeding women. Current guidelines indicate that pregnant individuals should only take Adderall if the benefits outweigh potential risks, highlighting the importance of consulting healthcare providers before making any decisions.
Can You Take Adderall While Pregnant? The Risks and Considerations
Using Adderall during pregnancy is a highly debated topic, and many healthcare professionals advise against it due to potential risks. The FDA classifies Adderall as a category C drug, which means that its effects on pregnancy are not fully understood but may pose risks to the fetus. It’s crucial to examine what we know about the potential impacts on pregnancy and fetal development.
Research indicates that amphetamines can cross the placenta, leading to concerns about fetal exposure during critical stages of development. Some studies have suggested that the use of stimulants during pregnancy may be associated with complications such as low birth weight, preterm birth, and potential neurodevelopmental issues. For example, a study published in the American Journal of Psychiatry found that there may be an increased risk of intrauterine growth restriction in fetuses exposed to ADHD medications, including amphetamines.
Moreover, pregnant women using Adderall may experience associated side effects such as appetite suppression, which can lead to insufficient weight gain for both mother and baby. Therefore, it is vital that expectant mothers work closely with their healthcare providers to evaluate their symptoms and discuss alternative treatment options if needed. In some cases, non-stimulant medications might be recommended to manage ADHD symptoms with fewer risks.
What Are the Alternatives for Managing ADHD Symptoms During Pregnancy?
If taking Adderall while pregnant is not advisable, what alternatives are available? Healthcare providers and mental health professionals often suggest a multi-faceted approach when it comes to managing ADHD during pregnancy. Therapies and lifestyle changes can be invaluable for many women. Some alternative options include:
- Cognitive Behavioral Therapy (CBT): This is a structured therapeutic approach that helps patients develop practical skills to manage their symptoms. It can be particularly effective for women who prefer to avoid medication during pregnancy.
- Mindfulness and Relaxation Techniques: Mindfulness-based interventions, yoga, and exercise can help improve focus and reduce anxiety, providing coping strategies without pharmaceutical intervention.
- Dietary Adjustments: Maintaining a balanced diet rich in omega-3 fatty acids, vitamins, and minerals can help support brain health and improve mood.
- Support Groups: Connecting with others who experience similar challenges can offer emotional support and practical advice.
Overall, collaborating with healthcare providers to tailor an appropriate treatment strategy is key for managing ADHD symptoms while pregnant.
Adderall and Breastfeeding: What You Need to Know
The question of whether to take Adderall while breastfeeding presents another layer of complexity. Similar to its effects during pregnancy, the use of Adderall while lactating also raises concerns due to the potential for amphetamines to pass into breast milk.
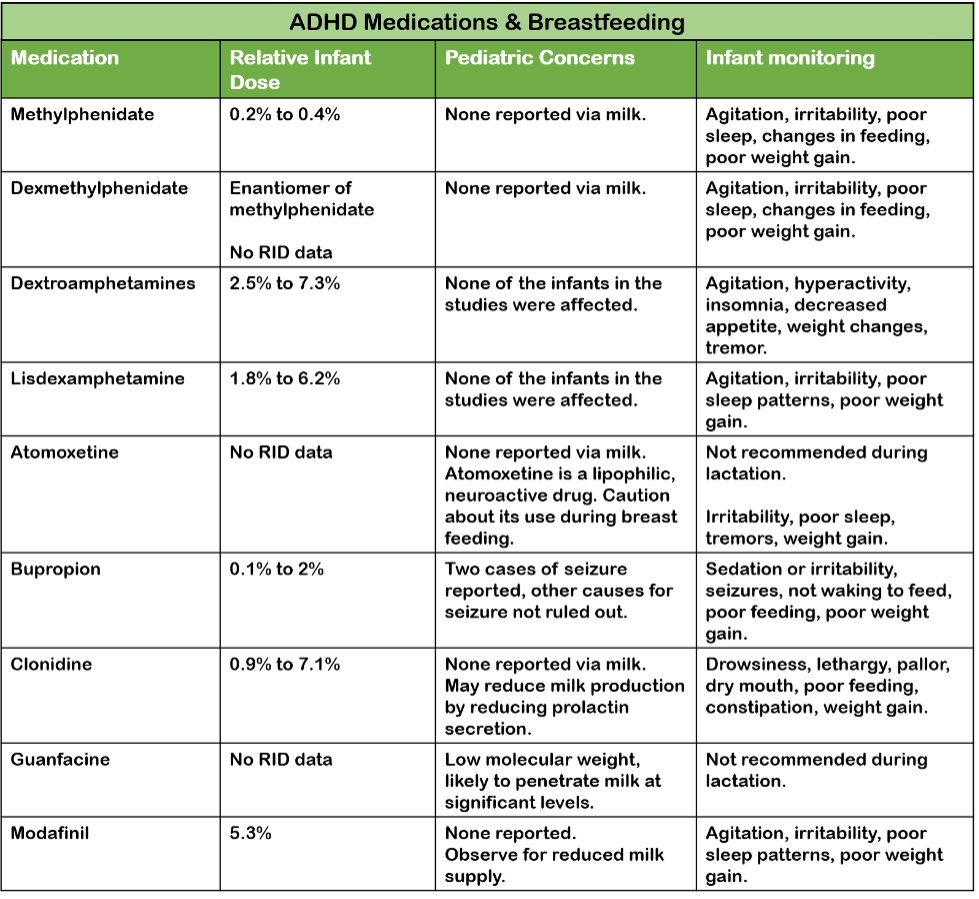
Research suggests that small amounts of the medication can be transferred to breast milk, which prompts caution. According to guidelines from organizations like the American Academy of Pediatrics, breastfeeding mothers should ideally avoid stimulant medications if possible. The MotherToBaby organization explicitly states that the product label for dextroamphetamine-amphetamine, commonly marketed as Adderall, recommends against its use for those who are breastfeeding.
However, many experts argue that the risks might be minimal for mothers taking lower doses of Adderall. Studies have indicated that the amount of amphetamines in breast milk is generally low—often less than 1% of the maternal dose. Reports suggest that infants exposed to low doses of amphetamines through breast milk do not exhibit negative effects on growth or development, particularly when mothers take under 45 mg per day.
Why Timing Your Doses Matters
One strategy that nursing mothers can consider is timing their doses of Adderall. For instance, taking medication immediately after breastfeeding can help minimize the amount of amphetamines present in breast milk when the infant nursed.
Breastfeeding mothers may benefit from working closely with their healthcare provider to find the right timing and dosage that balances their health needs with the safety of their baby. However, breastfed infants will require careful monitoring, especially if higher doses are involved. Regular pediatric check-ups can help ensure the child is developing healthily.
Real Experiences: Mothers Share Their Stories

Women’s experiences with ADHD medications during pregnancy and breastfeeding can vary widely, and many mothers have shared their stories online. The platforms like Reddit often feature discussions from mothers who took Adderall during various stages of pregnancy, some reporting successful management of their symptoms without adverse effects on their babies.
For example, a mother who took Adderall throughout her entire pregnancy noted that while she was initially concerned about potential risks, she closely monitored her son’s development and found that he was thriving. Another woman, who took low doses, recounted adjusting her ADHD treatment as her pregnancy progressed and ultimately found that therapy played a key role in managing her symptoms.
These anecdotal accounts, while not representative of all experiences, can provide insights into the challenges and outcomes faced by mothers in similar situations. It is important to emphasize that every individual’s experience is distinct, and consulting with healthcare providers is crucial when determining the appropriate treatment approach.
Understanding Common Concerns and Misconceptions
Several misconceptions circulate regarding the use of Adderall during pregnancy and breastfeeding. One significant concern is that using Adderall will inevitably result in negative effects on a child’s development. However, recent research indicates that low-dose usage, particularly in carefully monitored cases, may not significantly impact the child.
Another common misconception is the belief that all mothers will have to discontinue their ADHD medications upon discovering they are pregnant. Many healthcare providers emphasize that successful management of ADHD can often be achieved with alternative methods or careful dosing monitoring rather than complete cessation of medication.
Furthermore, the fear of stigma surrounding the use of stimulant medications can leave many mothers feeling isolated and anxious. Understanding that ADHD is a medical condition that can be managed effectively, even during pregnancy or breastfeeding, is vital for emotional well-being. Support from healthcare professionals, family, and peers can help empower mothers to make informed choices.
How Long Should You Wait to Breastfeed After Taking Adderall?
A widely asked question among nursing mothers is: how long should I wait to breastfeed after taking Adderall? This question largely depends on the dosage taken and the individual’s metabolism.
Research suggests that Adderall has a half-life of approximately 9 to 14 hours, meaning it generally takes this amount of time for half of the drug to exit the system. A common guideline is to wait approximately 4-6 hours before breastfeeding after taking a dose, which should help minimize the amount of medication transferred through breast milk. However, for mothers taking higher doses, extending this waiting period might be advisable.
While exact timing can vary for each individual, monitoring how a mother feels before breastfeeding can be an effective strategy. Additionally, consultation with a healthcare provider regarding specific circumstances can create a tailored plan that works best for both mother and baby, ensuring that the right measures are in place to facilitate safe nursing.
FAQs
1. Is taking a low dose of Adderall while pregnant safe?
The safety of taking a low dose of Adderall during pregnancy is not well established, and data suggest it is best avoided unless the benefits outweigh the risks. Pregnant women should consult with their healthcare providers to discuss alternative treatment options and assess the risks related to medication use carefully.
2. What should I do if I took Adderall before I knew I was pregnant?
If you took Adderall before discovering your pregnancy, it is advisable to consult your healthcare provider immediately. It is essential to discuss your concerns and potential risks while considering the best path forward for your health and the development of your baby.
3. Can I take 5mg of Adderall while breastfeeding?
A dose of 5mg of Adderall taken while breastfeeding may be less concerning than higher doses, but it is essential to monitor the infant for any unusual signs or symptoms. Consulting with your healthcare provider to develop a comprehensive care plan while monitoring breastfeeding is essential.
4. Are there any known long-term effects on children whose mothers took Adderall during pregnancy?
Current research on the long-term effects of children whose mothers used Adderall during pregnancy remains limited. Some studies indicate potential risks, but many children have developed healthily despite their exposure to amphetamines. Long-term follow-up by pediatricians is necessary to assess child development in these cases.
5. Are there any alternative treatments for ADHD during pregnancy?
Alternative treatments during pregnancy may include behavioral therapy, lifestyle modifications, and dietary changes that minimize symptoms of ADHD. Non-stimulant medications may also be viable options that can be explored with a healthcare provider to manage symptoms without associated risks.
6. What are the risks of not treating ADHD during pregnancy?
Failing to manage ADHD during pregnancy may lead to increased anxiety, insomnia, and impaired functioning, which can affect both the mother’s well-being and her ability to care for herself and her child. Carefully evaluating the risks of untreated symptoms is critical when discussing treatment options.
7. Can I take 10 mg of Adderall while breastfeeding?
Taking 10 mg of Adderall while breastfeeding should be discussed with a healthcare provider. The amount of medication that passes into breast milk is generally minimal, but monitoring the infant for any changes following maternal dose adjustments is important.
Conclusion: Navigating Medication Use During Pregnancy and Lactation
Deciding whether to take Adderall during pregnancy or breastfeeding is multifaceted, requiring thorough consideration of the associated risks and benefits. Women coping with ADHD find themselves at the intersection of managing their health while ensuring optimal outcomes for their babies. As we’ve seen, stimulant medications such as Adderall carry potential risks not only for the mother but also for the developing fetus and nursing infant.
Healthcare providers play a critical role in guiding expectant and breastfeeding mothers through this challenging landscape. By discussing alternative treatment options, monitoring infant development, and remaining informed about the implications of medication use, mothers can effectively navigate this complex situation. Ultimately, the key takeaway is to consult openly with healthcare professionals regarding individual circumstances, allowing for informed decisions tailored to personal health goals.
As knowledge about ADHD and its management continues to evolve, expecting mothers can take comfort in knowing that they are not alone during this journey. Resources are available to help mothers make empowered choices, facilitating a healthy relationship with themselves and their newborns while prioritizing both mental and physical well-being.

