🏠 Stay at home! 25% discount on all medicines
Is Ambien a Narcotic? Understanding its Classifications and Risks
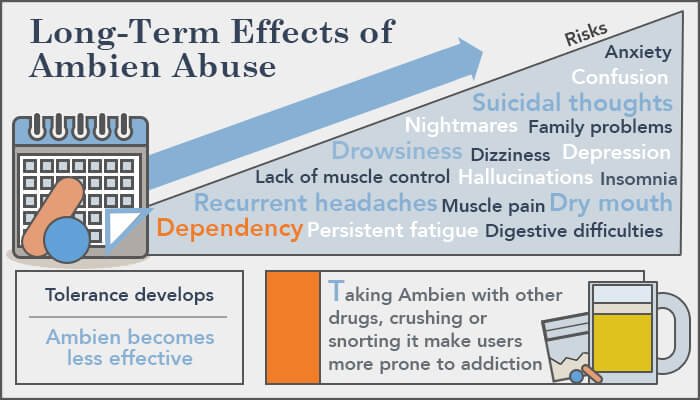
Ambien, known by its generic name zolpidem tartrate, is a popular medication primarily used to treat insomnia. In a world ravaged by sleep disorders, Ambien has provided relief to millions. However, there is a growing discourse around its classification, leading many to question: Is Ambien a narcotic? This question is crucial, especially as understanding drug classifications can impact not only potential users but also the medical community shaping treatment protocols.
Despite its sedative properties, Ambien does not fall under the narcotic category. The differentiation between narcotics and sedative-hypnotics is pivotal in understanding how this medication works within the body. Defining the potential risks, benefits, and underlying science behind Ambien will not only clarify its classification but also serve as an essential guide for its responsible use.
This article aims to dissect the nuances of Ambien’s classification, effect on the central nervous system, and overall implications of its use. Readers will gain a deeper understanding of Ambien’s role as a controlled substance, its function in sleep disorders, and the risks associated with its use—ultimately empowering them to make informed decisions about their health.

Understanding Ambien: A Comprehensive Overview
Ambien is predominantly prescribed for short-term management of insomnia. Since its approval in 1992 by the FDA, it has become a widely recognized solution for individuals struggling with falling asleep or staying asleep throughout the night. This sedative-hypnotic interacts with the brain’s neurotransmitter systems to facilitate sleep, influencing gamma-aminobutyric acid (GABA) receptors, which play a significant role in promoting relaxation and sleepiness.
Its effectiveness is underscored by its ability to induce sleep more quickly and enhance sleep quality, without many of the complications associated with traditional sleeping pills. The exact mechanism involves the modulation of neuronal activity at GABA receptors, which are inhibitory in nature and help calm brain activity. Even though Ambien is a powerful tool for sleep management, its classification can lead to misunderstanding among professionals and users alike.
The term ‘narcotic’ is often incorrectly applied to medications like Ambien. Traditionally associated with opiates and opioids used for pain management, the term narcotic denotes substances that can cause addiction, dependency, and other adverse effects. Ambien, despite its sedative-hypnotic capabilities, is not classified within this category—a significant point for those considering its use.
What Class of Drug Is Ambien?
Ambien is categorized under the drug class known as sedative-hypnotics, which are primarily designed to help patients with sleep disturbances. Sedative-hypnotics generally work by depressing the central nervous system, creating a calming effect that facilitates sleep onset. This class of drugs is essential for those struggling with sleep, especially for those diagnosed with chronic insomnia.
Although Ambien does share some similarities with narcotics—such as the potential for misuse and dependence—it lacks the specific characteristics that define narcotic substances like opioids. Instead, it belongs to a less rigid category governed by the U.S. Drug Enforcement Administration (DEA) as a Schedule IV controlled substance. This designation indicates that while there is a risk of abuse, it is significantly lower than that for other substances that fall under more stringent classifications.
Within the realm of sedative-hypnotics, Ambien is unique due to its rapid onset of action and relatively short half-life, which reduces the risk of residual next-day sedation. Contrarily, narcotics generally work through distinct pain-relieving pathways, often producing euphoria, which is a major factor in addiction. This essential difference emphasizes why understanding Ambien’s classification is crucial for effective and safe use.
How Does Ambien Work in the Body?
The mechanism of action for Ambien involves its interaction with the neurotransmitter GABA, which has significant implications for sleep regulation. By enhancing GABAergic activity in the brain, Ambien lowers neuronal excitability, leading to sedation and sleep inception for the user. The rapid absorption of this medication is one factor that distinguishes it from other sleep medications that may take longer to take effect.
Once ingested, Ambien enters the bloodstream and reaches peak levels in approximately 1.5 hours, leading to a prompt feeling of drowsiness. This is beneficial for patients who struggle with the initial phases of sleep onset. The calming effects of Ambien can be observed in both the reduction of sleep latency and the improvement of overall sleep quality, allowing for longer periods of uninterrupted sleep.
This rapid action can be a double-edged sword. While it offers immediate relief, the potential for misuse arises due to individuals seeking to use the drug for recreational purposes or to expedite sleep onset at inappropriate times. Consequently, patients are advised to take it only as prescribed and under professional guidance to mitigate risks associated with dependence and withdrawal.
Is Ambien a Controlled Substance?

Yes, Ambien is classified as a controlled substance under Schedule IV of the Controlled Substances Act, validated by the DEA. This classification is significant, primarily due to the implications regarding prescription protocols and the legal implications tied to its use. Schedule IV medications are monitored due to their potential for abuse and dependence, even though their risk profile is lower than that of substances placed in higher schedules.
Understanding the controlled substance classification implies that healthcare providers must evaluate patients thoroughly before prescribing Ambien, taking into account any history of substance abuse or coexisting mental health disorders. This step is crucial in mitigating the potential for abuse, which has been a growing concern with the increase in sleeping pill prescriptions.
The classification as a controlled substance also carries regulations concerning prescribing limits, refills, and the overall use of the drug within various healthcare settings. The focus on regulatory measures surrounding Ambien emphasizes the importance of safe use and monitoring by healthcare providers.
What Happens If Ambien Is Misused?
Misuse of Ambien can lead to several adverse effects, including dependence, withdrawal symptoms, and significant impairment in cognitive function and motor skills. Dependence can occur even with legitimate use as prescribed, as the body begins to adapt to the presence of the drug to the point of requiring it to function normally.
Withdrawal symptoms from Ambien can include severe insomnia, agitation, anxiety, and tremors, which may prompt individuals to return to using the drug, perpetuating a cycle of dependency. The potential for misuse further emphasizes the importance of responsibly managing prescriptions of Ambien through thorough patient education about its risks and benefits.
Additionally, misuse can manifest in dangerous behaviors, such as combining Ambien with other depressants or alcohol, which can lead to respiratory depression or overdose. Increased awareness among users regarding these potential dangers is critical in addressing misuse appropriately. The clear delineation between habitual and responsible use versus abuse is crucial for ensuring safety.
Ambien and Its Sedative Effects
As a sedative-hypnotic, Ambien works primarily by inducing sleepiness and promoting relaxation, making it a vital option for individuals experiencing acute or chronic insomnia. Unlike narcotics that primarily target pain relief, Ambien’s unique mechanism focuses on sleep regulation through modulation of GABA receptors, which directly influences neuronal excitability.
The sedative effects of Ambien facilitate a quicker transition into the various sleep stages, leading to increased periods of restful sleep. Particularly for those who face difficulties with sleep onset, Ambien offers a valuable solution that can result in profound benefits for overall well-being. Studies have consistently shown that improved sleep quality directly correlates with enhanced cognitive function, mood stabilization, and increased physical health.
However, while Ambien’s effectiveness as a sedative is well-documented, its side effects must be acknowledged. Common complaints among users include daytime drowsiness, impaired judgment, and potentialmemory lapses—often leading to concerns about next-day functioning. These factors necessitate a careful balance between the benefits of sleep induction and the risks of cognitive impairment and dependency.
Are There Alternatives to Ambien?
For individuals wary of potential side effects associated with Ambien, various alternatives are available for managing insomnia. Non-benzodiazepine medications, certain antidepressants, and over-the-counter options can offer effective solutions without the same class of risks that accompany sedative-hypnotics. Some patients may find success with lifestyle changes, such as cognitive behavioral therapy for insomnia (CBT-I), exercise, and relaxation techniques.
Herbal supplements like melatonin are also gaining popularity for their natural sedative effects, though their efficacy varies by individual. With an increasingly holistic approach to sleep management, it becomes essential to evaluate various options that promote healthy sleep patterns while minimizing the risk of dependency associated with prescription medications.
Patients considering alternatives should engage in open discussions with their healthcare providers, as they can guide appropriate strategies based on individual needs, preferences, and any concurrent medical conditions.
Ambien and Its Legal Status

Ambien is legal and available only through a prescription in countries like the United States. Its classification as a Schedule IV controlled substance means that it is subject to specific regulations regarding how it can be prescribed and dispensed. Patients must consult a qualified healthcare provider to discuss their symptoms and determine the most appropriate treatment options.
The regulatory framework surrounding Ambien is designed to ensure that it is used safely and effectively by those who need it. In recent years, increased awareness of substance misuse has led to stricter enforcement of prescribing guidelines, ensuring that healthcare providers remain vigilant regarding their prescribing practices.
Despite its legal status, individuals should practice responsibility in managing their prescriptions and avoid sharing medications. Misuse through sharing or incorrect dosing can create unnecessary health risks to others. It is incumbent upon individuals to understand the consequences of misuse regarding not just their own health but also the legal ramifications that accompany unauthorized distribution.
When Did Ambien Become a Controlled Substance?
Ambien was classified as a controlled substance in the United States shortly after its release in 1992. Specifically, it fell under Schedule IV due to concerns about misuse and the growing awareness of sleep medication’s potential for abuse. Since its initial introduction, there has been an increased focus on monitoring its use within healthcare settings and ensuring patient safety through responsible prescribing practices.
This development underscores the proactive measures that both health authorities and practitioners have taken to limit the risks associated with prescribing sedative-hypnotics while still providing solutions for those struggling with sleep. The recognition of Ambien as a controlled substance serves as a reminder of the importance of educating patients regarding potential risks and ensuring responsible use.
Healthcare systems continuously evaluate the status of medications based on evolving research and the prevalence of issues related to substance misuse, working to maintain the delicate balance between treatment efficacy and safety.
Exploring Ambien Addiction: Facts and Treatment Options
Although Ambien is not a narcotic, it does possess characteristics that can lead to addiction in certain individuals, predominantly due to its sedative effects and the potential for misuse. Understanding the warning signs of Ambien addiction is crucial for timely intervention and recovery.
Common symptoms of Ambien addiction include taking the medication in ways not prescribed, experiencing cravings, and continuing to use the drug despite resulting adverse consequences such as cognitive impairment or increased anxiety. Being aware of these symptoms is essential for patients and their loved ones to address issues of dependence before they escalate.
Treatment for Ambien addiction typically involves a combination of detoxification and behavioral therapy aimed at addressing the underlying issues that prompted the use of the drug. Cognitive-behavioral therapy (CBT) has proven effective in helping individuals modify their thought patterns and behaviors associated with substance misuse. Support groups and rehabilitation programs further empower individuals by providing community-level support during their recovery journey.
Preventing Ambien Addiction
Preventing Ambien addiction requires collaborative efforts between healthcare providers and patients. Open communication regarding dosage, duration of use, and the potential for dependence must be emphasized during initial consultations. Establishing clear prescriptions and monitoring usage can significantly mitigate the risks associated with this medication.
Patients are encouraged to adhere strictly to the prescribed instructions, avoid self-medicating, and communicate any changes in their health status or side effects to their healthcare provider. Establishing a strong support network among family and friends can also enhance accountability and aid in recognizing concerning behaviors early on.
Furthermore, patients should explore all available treatment options, considering non-pharmacological alternatives to management of insomnia that may pose less risk for dependency. Through education and awareness, patients can better navigate their treatment, maximizing the therapeutic benefits of Ambien while minimizing the potential for adverse consequences.
FAQ: Common Questions About Ambien
Is Ambien a benzodiazepine?
No, Ambien is classified as a sedative-hypnotic medication, not a benzodiazepine. While both classes of medications can be used for similar purposes, such as managing anxiety or insomnia, benzodiazepines act primarily on the central nervous system through GABA receptors and possess a wider range of indications. Ambien’s therapeutic use is specifically indicated for short-term treatment of insomnia, making it distinctly different from benzodiazepines.
How long does Ambien stay in your system?
The half-life of Ambien is approximately 2.5 hours, meaning that it typically stays in your system for around 24 hours after ingestion. However, the duration can vary based on individual factors, including metabolism, age, and concurrent medications. While its effects may subside after a few hours, it is essential to refrain from activities requiring full attention and coordination, such as driving, when taking Ambien.
Can you drink alcohol while taking Ambien?
Combining alcohol with Ambien is highly discouraged due to the significant risk of respiratory depression and increased sedation. Both substances exert depressant effects on the central nervous system, which can lead to heightened drowsiness and impaired judgment. Therefore, individuals using Ambien should avoid alcohol entirely to ensure their safety and adhere to prescribed guidelines.
What are the side effects of Ambien?
Common side effects of Ambien may include drowsiness, dizziness, headache, and gastrointestinal disturbances. More serious side effects could involve complex sleep behaviors, such as sleepwalking or unusual behaviors directed towards eating and driving during sleep, without any conscious awareness of these actions. Patients should report any troubling symptoms to their healthcare provider, who can adjust the treatment protocol as necessary.
Is it safe to take Ambien long-term?
Long-term use of Ambien is generally not recommended due to the potential development of tolerance, dependence, and withdrawal symptoms. Healthcare providers typically prescribe it for short-term use (a few weeks) only, followed by careful monitoring for re-emergence of insomnia symptoms. Patients should engage in discussions with their healthcare providers to address chronic sleep issues responsibly and explore alternative therapies.
Can Ambien cause nightmares?
Some users of Ambien report experiencing vivid dreams or nightmares as a side effect. These occurrences may be attributed to the medication’s action on the central nervous system, which alters normal sleep architecture. While this is relatively uncommon, patients experiencing disturbing dreams should consult their healthcare provider to explore potential adjustments to their treatment regimen.
Conclusion: Navigating Ambien Responsibly
Understanding whether Ambien is a narcotic necessitates an exploration of its classification and potential implications for users. While Ambien does not fall under the narcotic category, it does present risks commonly associated with controlled substances, reinforcing the need for responsible use and monitoring.
Ambien’s role as a sedative-hypnotic provides a valuable tool for managing sleep disorders, emphasizing the need for an informed approach to its utilization. Users must be aware of the differences between narcotics and sedative-hypnotics, ensuring that they establish clear channels of communication with their healthcare providers regarding usage and any concerns surrounding its effects.
With a collaborative mindset, patients can maximize the benefits of medications like Ambien while minimizing risks, ultimately paving the way for a better understanding of sleep health management. In a world increasingly focused on holistic well-being, responsible use of medications remains essential in promoting optimal health outcomes.

