🏠 Stay at home! 25% discount on all medicines
How Does Adderall Work: Unveiling the Mechanism Behind the Popular Stimulant
Adderall, a medication often prescribed to treat Attention Deficit Hyperactivity Disorder (ADHD), has gained immense popularity over the years. With increasing numbers of adults seeking prescriptions for cognitive enhancement, understanding how Adderall works in the brain and body is more crucial than ever. Whether you’re considering Adderall for ADHD treatment or are merely curious about its effects on cognition and mood, the science behind it is both fascinating and complex.
Statistics reveal that ADHD affects approximately 5% of children and often continues into adulthood, where it impacts about 2.5% of adults. With such widespread prevalence, the demand for effective treatments like Adderall has surged. But beyond its therapeutic uses, many are intrigued by how this powerful stimulant interacts with the brain. This article will delve deeply into the mechanisms of Adderall, highlighting its effects on neurotransmitter levels, the implications for those with and without ADHD, and the associated risks and benefits.
By the end of this comprehensive guide, you will gain a thorough understanding of how Adderall functions at both a chemical and behavioral level. We will discuss its effects on the brain, its efficacy in ADHD treatment, and what individuals may experience when taking it—whether they have ADHD or not. The landscape of ADHD treatment is complex, and knowledge about medications like Adderall is essential for informed discussions undoubtedly beneficial to both patients and healthcare providers.

How Adderall Works in the Brain
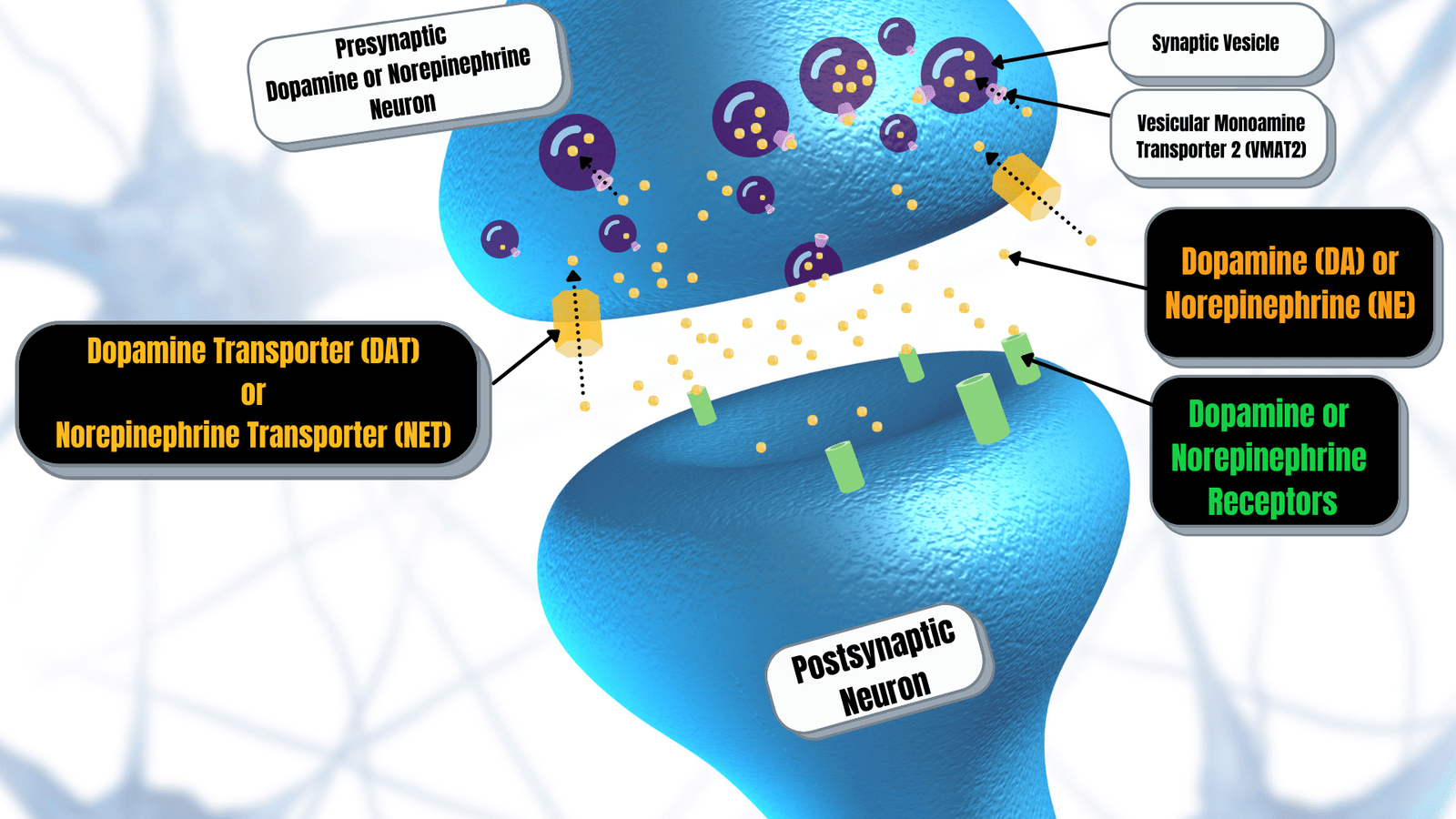
To comprehend how Adderall works, it is essential to first understand the structure and function of the brain. Central to Adderall’s action is its influence on neurotransmitters—chemical messengers that transmit signals across synapses. The primary neurotransmitters affected by Adderall are dopamine and norepinephrine. These neurotransmitters play pivotal roles in mood regulation, attention, and overall cognitive function.
Adderall is classified as a central nervous system (CNS) stimulant, predominantly used to increase the levels of dopamine and norepinephrine in the brain. When Adderall is ingested, it stimulates the release of these neurotransmitters, promoting neurotransmission in areas of the brain responsible for attention and executive functioning. Specifically, Adderall influences the prefrontal cortex, which is crucial for maintaining attention, focus, and impulse control.
Moreover, research indicates that the increase in dopamine levels enhances feelings of satisfaction and reward, which can improve motivation and engagement in tasks. This mechanism not only enhances cognitive function for individuals with ADHD but also extends to improve attention and focus among people without ADHD, leading to its misuse for cognitive enhancement among students and professionals.
What Chemical Processes Are Involved?
Adderall’s chemical structure consists of a combination of amphetamine salts. Upon ingestion, it interferes with the reuptake of dopamine and norepinephrine at the synapse. By blocking the transporters responsible for their reabsorption, Adderall allows these neurotransmitters to linger in the synaptic cleft longer than they normally would. This increased availability boosts signaling between neurons and enhances their effects on attention and focus.
Furthermore, Adderall prompts an increased release of dopamine from the presynaptic neurons, leading to heightened arousal and alertness. Particularly in patients diagnosed with ADHD, this stimulation can correct neurotransmitter deficiencies that contribute to the symptoms of the disorder. The acute onset of effect typically occurs within 30 minutes of administration, with peak concentrations experienced within 1 to 3 hours.
Another significant aspect of Adderall’s action pertains to its effect on norepinephrine, which relates closely to the brain’s response mechanism during stressful situations. By amplifying norepinephrine release, Adderall can enhance alertness, attention, and responses to stimuli, inducing a state often referred to as “hyperfocus” in those with ADHD.
How Does Adderall Affect Neurotransmitter Levels?
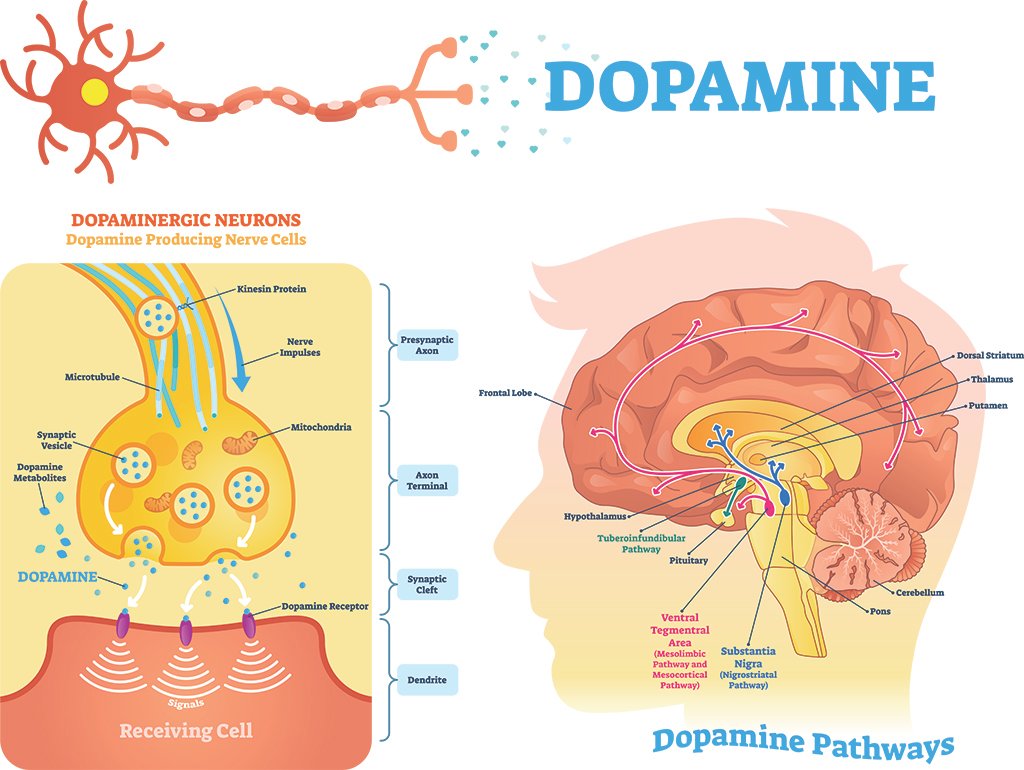
The modulation of neurotransmitter levels intricately ties back to the core functionalities of Adderall. Research indicates that individuals with ADHD often experience a deficiency in dopamine transmission, primarily in the mesolimbic and mesocortical pathways. Adderall addresses this deficit, providing a more balanced state of neurotransmission.
The typical range of normal dopamine levels is critical for natural decision-making processes and executive function. When Adderall raises dopamine levels, it allows for better modulation of attention, increased impulse control, and an overall enhancement in cognitive functions. However, it’s essential to note that this should be done under medical supervision, as misuse or overdosage can lead to significant health risks.
Conversely, Adderall’s effects are starkly different for individuals without ADHD. While they can also experience enhanced focus and alertness, the accompanying euphoria can lead to a potential risk of abuse and dependency. The distinct reaction in these individuals highlights the fine line between therapeutic use and recreational misuse.
The Effects of Adderall on People with ADHD
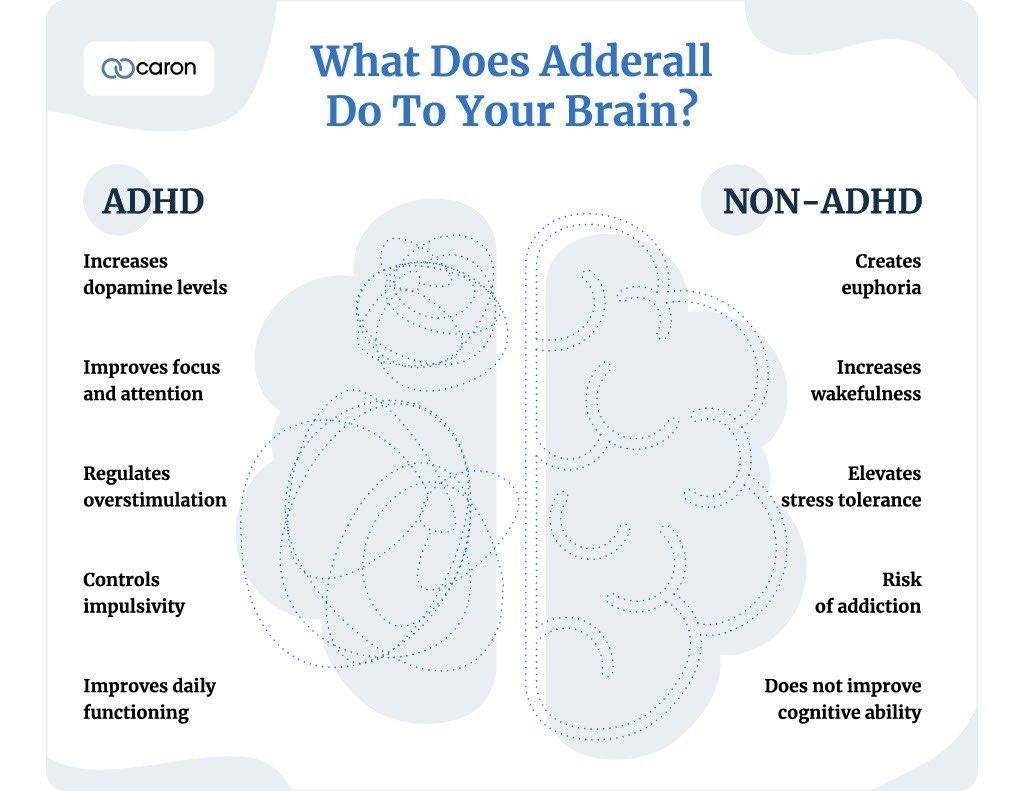
For individuals diagnosed with ADHD, Adderall serves a pivotal role in managing symptoms. The medication is designed to correct the neurochemical imbalances that characterize the disorder, ultimately aiding better attention span, improved organization skills, and heightened impulse control. However, understanding its therapeutic effects needs a closer look at how they manifest in practical scenarios.
One notable benefit is the improvement in academic performance among children and adults with ADHD. The enhanced focus allows for better engagement in classroom settings and increased productivity in work environments. Studies show that students prescribed Adderall exhibit improved grades and heightened attention spans during lessons compared to their non-medicated peers.
Moreover, the medication helps in regulating emotional responses. Individuals with ADHD often experience emotional dysregulation, leading to frustration and outbursts. Adderall can aid in tempering these responses, promoting overall emotional stability. However, consistent monitoring by healthcare professionals is recommended to ensure that the benefits continue while minimizing potential side effects.
How Long Does Adderall Stay in the System?
The duration of Adderall’s effects can vary based on its formulation. Typically, Immediate Release (IR) formulations last around 4 to 6 hours, while Extended Release (XR) forms can remain effective for up to 12 hours. The half-life—the time it takes for half the drug to be eliminated from the body—ranges from 9 to 14 hours depending on individual metabolism and the specific formulation used.
Various factors influence how long Adderall remains in the system. For instance, hydration levels, body mass, and frequency of use can all impact elimination rates. Chronic users may develop tolerance, requiring higher doses to achieve the same effect, and this can also alter how long the drug functions effectively in the system.
Since Adderall is addictive in nature, understanding its pharmacokinetics and monitoring its duration of action is critical for those who use it. Regular consultations with healthcare providers are essential for adjusting dosages and avoiding potential long-term side effects.
Potential Side Effects in Individuals with ADHD
While Adderall is effective for many, it is not devoid of side effects. Commonly reported effects include insomnia, dry mouth, loss of appetite, and increased anxiety. In some cases, patients may also experience cardiovascular side effects, such as increased heart rate and blood pressure. Standard practices dictate monitoring these parameters during treatment to ensure patient safety.
Long-term use and dosage considerations must also factor into the decision to use Adderall. Excessive use can lead to more severe side effects, including potential addiction, withdrawal symptoms upon discontinuation, and risk of mental health issues such as depression and anxiety. Thus, it is imperative for patients to adhere to prescribed dosages and maintain an open dialogue with their healthcare professionals.
Another significant concern is the potential for misuse, particularly among those who do not have ADHD. The stimulating effects can lead to euphoric feelings, driving some individuals to misuse the medication for cognitive enhancement or recreational purposes.
How Does Adderall Work on People Without ADHD?
The appeal of Adderall stretches beyond individuals with ADHD, particularly within academic and professional circles. Many non-ADHD individuals turn to Adderall with the hopes that it will increase their focus, productivity, and cognitive performance. Understanding how Adderall affects these individuals reveals a blend of both potential benefits and significant risks.
In individuals without ADHD, Adderall tends to produce effects such as increased alertness, energy, and possibly, a temporary improvement in cognitive tasks. Many users report heightened concentration for extended periods, making it appealing for students facing tight deadlines or professionals managing heavy workloads. Clinical studies suggest that these cognitive enhancements can occur even in healthy adults, albeit with varying degrees of effectiveness depending on individual neurochemistry.
However, the immediate effects can also be accompanied by adverse consequences. Non-ADHD users may experience heightened anxiety, jitteriness, and insomnia, as the drug may overstimulate their systems. The potential for increased heart rate and blood pressure is markedly concerning, particularly for those with pre-existing health conditions. The risk for dependency is also significant; the euphoric effects may lead individuals to misuse or abuse the drug in pursuit of heightened performance.
Does Adderall Make You High?
A critical question surrounding Adderall, especially among those considering its use for cognitive enhancement, is whether it can induce a “high.” The short answer is nuanced; while it does not produce the same euphoric sensation as other stimulants or drugs, Adderall can impart feelings of increased energy and alertness. This sensation mimics a form of mild euphoria, but it is contingent on individual neurochemistry.
For individuals with ADHD, the effects can feel stabilizing, allowing for focused productivity, whereas those without ADHD might experience an unsustained high that can lead to overactivity and subsequent crashes as the medication wears off. Hence, the line between therapeutic effects and potential addiction can become blurred.
This is further complicated by how Adderall is regulated. It is classified as a Schedule II controlled substance due to its potential for misuse and dependency. As such, illicit use among non-prescribed individuals poses significant legal and health risks.
Risks and Considerations of Adderall Use
Despite its effectiveness in treating ADHD and its appeal for cognitive enhancement, Adderall is accompanied by various risks. Being a stimulant, it has the potential for addiction and misuse, especially among individuals misusing it for academic or professional performance boosts. The consequences of prolonged use can also extend beyond dependency; they can lead to cardiovascular issues, insomnia, and mental health disorders. Thus, caution is paramount.
Regardless of whether an individual is using Adderall for legitimate medical reasons or to enhance performance, consideration of side effects is crucial. Patients are encouraged to remain in close contact with healthcare providers to monitor any emerging issues and adjust treatment protocols as necessary.
The risks of adverse effects are amplified when individuals purchase Adderall illegally. Recreational users are often unaware of the specific components in counterfeits, which may lead to further health complications. For example, dosages may not be regulated, creating scenarios of unintentional overdose or exposure to harmful substances.
Ways to Mitigate Adderall Risks
For individuals prescribed Adderall, one of the best ways to mitigate risks is to adhere strictly to a doctor’s orders. Regular consultations with mental health professionals are recommended to monitor progress and any side effects experienced during treatment. This transparent communication can lead to adjustments in dosage or change in treatment strategies if necessary.
Managing lifestyle choices can also influence the effectiveness and minimize the side effects of Adderall. Consuming a well-balanced diet, regular exercise, and maintaining proper sleep hygiene can facilitate a more stable response to the medication. Proper hydration is also vital, as dehydration can exacerbate several side effects, including dry mouth and insomnia.
For those considering Adderall for enhancement purposes, individuals should remain conscious of the research surrounding potential side effects and the danger of dependency. Seeking alternatives for cognitive improvement, such as lifestyle and behavioral changes, may yield better long-term outcomes without associated risks.
Understanding Adderall’s Impact on Everyday Life
For many individuals navigating life with ADHD, the introduction of Adderall can feel like a transformative experience. The ability to focus without distraction, manage time effectively, and regulate emotions offers significant improvements in academic and social contexts. However, this medication can also change how relationships and day-to-day interactions are approached.
For parents of children with ADHD, monitoring how Adderall influences their child’s behavior can provide insights into both positive and negative aspects. Improvements often manifest as better performance in school, while potential side effects, such as mood swings or irritability, could raise concerns. Communication among parents, teachers, and counselors remains vital in assessing the child’s overall progress.
For adults, understanding how Adderall affects their work-life balance is equally significant. While better focus and productivity are observable benefits, individuals should also recognize the importance of maintaining boundaries and practices to avoid burnout. Finding a healthy balance between work obligations and personal time is essential for sustained well-being.
How to Communicate with Your Healthcare Provider
The relationship between patients and healthcare providers is crucial for successfully navigating the complexities of Adderall treatment. Individuals are encouraged to discuss their experiences candidly, including any negative side effects or concerns about dependency. Monitoring tools, such as journals tracking usage and effects, can also aid discussions regarding effectiveness and risks associated with Adderall.
Additionally, it may be beneficial to explore alternative treatment options, particularly as lifestyle changes can positively influence ADHD symptoms. Behavioral therapy and coaching are valid alternatives that can complement or substitute the need for pharmacological interventions.
Ultimately, clear communication will allow for tailored approaches to treatment and greater satisfaction with the management of ADHD symptoms.
FAQ Section
What are the common side effects of Adderall?
Common side effects of Adderall include insomnia, dry mouth, decreased appetite, and increased heart rate. Other potential effects may involve increased anxiety and mood changes. Regular monitoring is advisable to address any adverse effects.
Can Adderall be addictive?
Yes, Adderall has the potential for addiction, especially when misused or taken in higher doses than prescribed. It is classified as a Schedule II controlled substance, indicating a high potential for misuse. Responsible use under medical supervision is critical to mitigating this risk.
How long does it take for Adderall to work?
Adderall’s effects typically begin within 30 minutes of ingestion, with peak effectiveness seen between 1 to 3 hours after consumption. The duration of action can vary based on whether the immediate or extended-release formulation is used.
Is it safe to take Adderall without a prescription?
No, taking Adderall without a prescription poses significant health risks. Illicit use can lead to severe side effects, increased risk of dependency, and legal consequences. Only individuals diagnosed with ADHD or other legitimate conditions should use this medication under healthcare supervision.
What should I do if I experience negative side effects from Adderall?
Patients experiencing negative side effects from Adderall should communicate with their healthcare provider immediately. Adjustments to dosage or switching medications might be necessary to mitigate adverse effects while continuing effective treatment.
How does Adderall affect people without ADHD?
For people without ADHD, Adderall may induce increased alertness and focus; however, it can also lead to heightened anxiety, jitteriness, and potential dependency due to its stimulating effects. Responsible use is highly advised.
Can lifestyle changes improve ADHD symptoms without medication?
Yes, lifestyle changes such as a balanced diet, regular exercise, sufficient sleep, and behavioral therapies can effectively manage ADHD symptoms. Many individuals find that a multi-faceted approach yields the best outcomes, sometimes reducing the need for medication.
Conclusion
Understanding how Adderall works offers critical insights into its efficacy, risks, and the broader implications for individuals diagnosed with ADHD. As a powerful stimulant, Adderall provides significant benefits when used appropriately, enhancing attention, focus, and emotional regulation in patients. However, its potential for misuse and abuse highlights the importance of cautious application.
For individuals without ADHD, the risks associated with Adderall use necessitate thorough consideration. While it may offer temporary cognitive enhancements, dependency and adverse side effects underscore the need for responsible management. Ultimately, fostering open conversations between patients and healthcare providers leads to more successful treatments and healthier approaches to both ADHD management and cognitive enhancement.
As the landscape of ADHD treatment continues to evolve, an informed approach to medications like Adderall, combined with lifestyle changes and behavioral strategies, provides a holistic framework for addressing symptoms and achieving long-term success. Whether considering Adderall for therapeutic use or as a cognitive enhancer, understanding its mechanisms will empower individuals to make informed decisions.

