🏠 Stay at home! 25% discount on all medicines
Is Adderall a Controlled Substance? Understanding Its Classification and Implications
In the realm of prescription medications, few are as widely discussed and debated as Adderall. Originally developed in the 1920s for various medical conditions, it has gained notoriety as a focus-enhancing drug, particularly within academic centers and workplaces. However, a critical question persists: is Adderall a controlled substance?
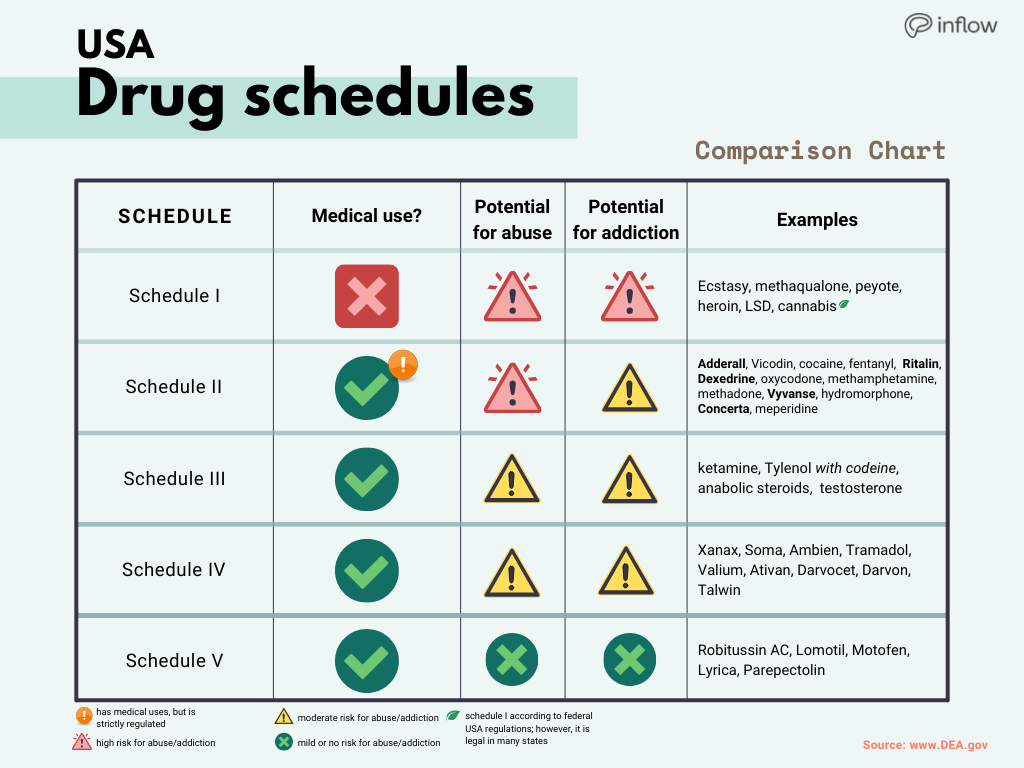
According to the U.S. Drug Enforcement Agency (DEA), Adderall is officially classified as a Schedule II controlled substance. This designation is significant, as it categorizes medications based on their accepted medical uses and potential for abuse. Understanding what this classification means is essential for patients, healthcare providers, and society at large.
This article will unpack the complexities of Adderall’s classification, examining its usage, potential for abuse, legal implications, and the societal impact of this medication. By the end, readers will have a comprehensive understanding of the risks and responsibilities associated with Adderall and similar medications.

What Does It Mean for Adderall to Be a Controlled Substance?
To grasp the implications of Adderall’s classification, it is essential to understand the regulatory framework that governs controlled substances in the United States. The Controlled Substances Act (CSA) divides drugs into five schedules based on their medical utility and potential for abuse.
As a Schedule II controlled substance, Adderall is recognized as having legitimate medical applications, primarily for treating Attention Deficit Hyperactivity Disorder (ADHD) and narcolepsy. However, it is also associated with a high potential for misuse and addiction. This classification reflects both its therapeutic benefits and the serious risks it poses to users.
The labeling of Adderall as a controlled substance impacts various aspects of its availability and usage. Healthcare providers must adhere to strict regulations when prescribing it, including requiring written prescriptions and monitoring patient use. Additionally, patients face restrictions on how many refills they can receive, requiring more frequent visits to their healthcare provider for continued therapy.
Why Is Adderall Classified as Schedule II?
Adderall’s classification stems from its chemical composition and effects on the central nervous system. It contains a combination of amphetamine salts that stimulate brain activity, enhancing focus and concentration, which can lead to significant improvements in individuals with ADHD.
However, the same properties that make Adderall effective for treating ADHD also render it susceptible to misuse. Reports indicate that many individuals, particularly students, seek out Adderall as a means to enhance cognitive performance or combat fatigue. This form of non-prescribed usage dramatically increases the risk of addiction and dependence.
The combination of its legitimate therapeutic uses alongside the potential for recreational misuse solidifies Adderall’s position as a Schedule II drug. As such, it is subject to rigorous regulatory scrutiny to prevent diversion and abuse.
The Risks of Using Adderall Without Prescription

The allure of Adderall often stems from its reputation as a cognitive enhancer, particularly among students in high-pressure academic environments. However, using Adderall without a prescription poses several risks that can profoundly affect an individual’s physical and mental health.
Adderall misuse can lead to serious side effects, including cardiovascular complications, anxiety, and stimulant use disorder. Adderall works by increasing dopamine levels in the brain, which can create a pleasurable experience for users; this increase, while effective for managing ADHD symptoms in prescribed doses, can lead to dangerous outcomes when higher doses are self-administered.
Furthermore, the use of Adderall can lead to psychological dependency. Users may find themselves needing to take higher doses over time to attain the same effects or may experience significant withdrawal symptoms when they cease use. These factors contribute to the drug’s reputation for abuse and its classification as a controlled substance.
How Prevalent Is Adderall Abuse?
Statistics reveal substantial rates of Adderall misuse, especially among college students. Research indicates that approximately 30% of college students have misused prescription stimulants like Adderall at some point during their academic careers. These figures underscore the need for awareness and education surrounding the risks associated with non-medical use of this medication.
Moreover, surveys show that nearly one in four college students meet the medical criteria for substance abuse, underscoring the urgent issue of stimulant misuse on campuses nationwide. While many individuals believe they can handle these substances without consequences, the reality is that the risks associated with Adderall demand serious consideration, especially for young adults in academic environments.
Legal Implications of Adderall’s Classification
The legal landscape surrounding Adderall is shaped heavily by its classification as a Schedule II controlled substance. This designation imposes strict regulations on how the drug can be prescribed, dispensed, and possessed.
In many jurisdictions, possession of Adderall without a valid prescription can lead to severe legal consequences, including criminal charges. Laws vary by state; for instance, in Texas and Florida, laws surrounding controlled substances are particularly stringent, reflecting the seriousness with which jurisdictions view the abuse potential of medications like Adderall.
Furthermore, healthcare providers must navigate a complex web of rules when prescribing Adderall. Prescribers are required to assess patients rigorously and must implement appropriate monitoring to mitigate the risk of abuse. Failure to comply with these regulations can lead to legal repercussions for both the provider and the patient.
Differences in State Regulations
The regulations governing Adderall can vary significantly from state to state. While all states recognize Adderall as a Schedule II controlled substance, states like Texas and Florida may have additional criteria for prescribing and monitoring its use. For example, in Texas, healthcare providers are encouraged to utilize the Prescription Monitoring Program (PMP) to track prescriptions for controlled substances, including Adderall. This program helps identify potential misuse patterns and curb diversion.
In Florida, laws have become even stricter, particularly following the state’s struggle with prescription drug abuse. Here, prescribers may face heightened scrutiny regarding their prescribing practices, especially for controlled substances such as Adderall.
Can Adderall Be Prescribed Safely?

Despite its potential for abuse, when prescribed appropriately and monitored closely, Adderall can be safely used as part of a comprehensive treatment plan for ADHD. Medical professionals are trained to recognize the signs of substance misuse and can implement guidelines to minimize risks while maximizing therapeutic outcomes.
A crucial component of safe prescribing involves thorough patient evaluation, including a detailed medical history and current health assessment. Clinicians are encouraged to engage in ongoing dialogue with patients regarding their treatment plans, as well as any concerns or changes in symptoms.
Additionally, regular follow-ups are vital for monitoring dosage and assessing effectiveness. This holistic approach not only supports patient safety but also enhances the overall treatment experience for those affected by ADHD.
What Are Alternative Treatments to Adderall?
For individuals seeking alternatives to Adderall, several options exist. Non-stimulant medications, such as atomoxetine and guanfacine, can offer effective treatment for ADHD without the same potential for abuse. These medications work differently than stimulants, targeting specific neurotransmitters to manage symptoms.
Behavioral therapies, including Cognitive Behavioral Therapy (CBT), can also play a vital role in managing ADHD symptoms. These therapeutic interventions focus on developing coping strategies and addressing negative thought patterns, providing individuals with tools that promote effective self-management without reliance on medication.
Addressing Common Misconceptions about Adderall
Numerous myths surrounding Adderall impede understanding of its true nature and risks. One prevalent misconception is that because Adderall is a prescribed medication, it is inherently safe for anyone to use, given their perceived needs. This misunderstanding can lead to misuse, as individuals justify taking the drug based on anecdotal evidence from others.
Another common belief is that stimulant medications are not addictive. While they can be safely used under medical supervision, the potential for addiction is real and significant, emphasized by the drug’s Schedule II classification. Many individuals underestimate the seriousness of this risk, believing they can use the drug without adverse consequences.
How Does Adderall Affect Different Populations?
The effects of Adderall can vary significantly across different populations. For individuals diagnosed with ADHD, the medication can lead to improved concentration and focus, significantly enhancing their quality of life. However, without an ADHD diagnosis, individuals taking Adderall may experience extreme side effects, including heightened anxiety, insomnia, and cardiovascular complications.
Moreover, the young adult demographic, particularly college students, often feels pressure to perform academically, which can lead to a higher likelihood of using the drug non-medically. This group may not fully recognize the risks involved, nor do they fully understand how Adderall can affect their bodies compared to those for whom it has been prescribed medically.
Staying Informed: Empowering Yourself on Prescription Use
Empowerment through knowledge is crucial for understanding the complexities surrounding prescription medications like Adderall. Patients must engage in open communication with their healthcare providers about the potential risks, benefits, and concerns involving their medications.
Furthermore, individuals should remain informed about regulations governing controlled substances in their specific states to navigate their treatment effectively. Awareness can serve as a protective factor against potential misuses and ensure compliance with legal frameworks.
For those prescribed Adderall, attending regular follow-up appointments and participating in medication management programs can foster a safe treatment experience, enhancing both health outcomes and psychological well-being.
FAQs about Adderall and Controlled Substances
1. Is Adderall considered a narcotic?
No, while Adderall is classified as a controlled substance due to its potential for abuse, it is not a narcotic. Narcotic drugs generally pertain to opioids that are used for pain relief, whereas Adderall falls under the category of stimulants that enhance energy and focus.
2. What Schedule is Adderall classified under?
Adderall is classified under Schedule II of the Controlled Substances Act, indicating that it has a recognized medical use but also a high potential for abuse and dependency. This classification imposes stringent regulations on prescribing and dispensing the medication.
3. What happens if you possess Adderall without a prescription?
Possessing Adderall without a valid prescription can result in serious legal consequences, including criminal charges. Specifically, under Health and Safety Code 11350 HS, being caught with Adderall can lead to misdemeanor or felony charges, depending on the circumstances.
4. Can you become addicted to Adderall?
Yes, Adderall has a potential for addiction, particularly when misused. When taken in higher doses or without a prescription, individuals may develop tolerance and experience withdrawal symptoms upon cessation, indicating physical dependence.
5. How can I tell if Adderall is affecting my mental health?
Monitoring changes in mood, anxiety levels, and overall mental well-being is essential. If you notice heightened anxiety, feel overly stimulated, or experience significant changes in behavior while taking Adderall, it is crucial to discuss these changes with a healthcare professional.
Conclusion
Understanding the complexities surrounding Adderall as a controlled substance is crucial for anyone considering its use or currently prescribed the medication. Given its status as a Schedule II drug, Adderall carries significant implications for both legal and health-related aspects of usage.
As with any prescription medication, there are benefits as well as risks that must be carefully weighed. Patients and healthcare providers must engage in open and ongoing dialogue to ensure that treatment plans prioritize safety while addressing the individual needs of those affected.
For individuals navigating ADHD or seeking cognitive enhancement, being informed and responsible about medication usage will promote healthier lives that aren’t overshadowed by the risks associated with substance misuse. Empower yourself with knowledge, communicate with your healthcare provider, and understand that the journey to managing symptoms of ADHD is more than just medication—it’s part of a comprehensive treatment strategy that includes lifestyle interventions, monitoring, and support.

